June 20, 2000
TO: Each Supervisor
FROM: Mark Finucane
Director of Health Services
SUBJECT: DRAFT TOBACCO SETTLEMENT AGREEMENT PLAN
The enclosed draft entitled “Master Tobacco Settlement Funds for Los Angeles County: An Opportunity to Improve the Health of County Residents” supercedes the earlier draft we forwarded to you on February 28, 2000. The major change is an adjustment of recommended allocations based on a reduction of the estimated average annual installment from $130 million/year to $105 million/year based on the latest estimates from the Attorney General's Office.
This plan is based on certain assumptions that may not be applicable given the continuing Waiver discussions and the plan will most likely be amended to reflect future funding decisions over the next several weeks, including a re-examination of funding priorities identified by the Department of Mental Health.
If you have any questions or need additional information prior to our presentation of this plan, please let us know.
MF:al
Enclosure
c: Chief Administrative Officer
County Counsel
Executive Officer, Board of Supervisors
· Prevention of Serious Health Risks and Health Conditions Page 12
· Early Diagnosis and Treatment of Remediable Problems Page 15
· Enhancing the Open Door/Safety Net System Page 17
· Strengthening Capacity and Health Protection Systems Page 19
Master Tobacco Settlement Funds for Los Angeles County:
An Opportunity to Improve the Health of County Residents
Introduction
This plan is in response to the Board of Supervisors’ (Board) directive to develop recommended spending priorities for the Master Tobacco Settlement funds. It is estimated that Los Angeles County will receive $2.7 billion over the next 25 years—an average of about $105 million per year. This revenue stream represents an unprecedented opportunity to integrate tobacco control and other disease prevention and health promotion priorities into an overall plan to improve the health of County residents. This significant amount of funding also constitutes a challenge to make wise investment decisions about its expenditure for existing and new health programs that maximize return in terms of the health of our population.
In November 1998, Attorneys General and representatives of 46 states, the District of Columbia and five territories signed an agreement with the five largest tobacco manufacturers ending a four-year battle. The agreement settled all antitrust, consumer protection, common law negligence, statutory and restitutionary relief alleged by any of the states and territories signing the agreement. The major components of the Master Tobacco Settlement Agreement are:
· states receive $206 billion over 25 years;
· industry funds public education fund of $1.45 billion;
· industry pays $250 million, over ten years, to fund a charitable foundation to study programs to reduce teen smoking and substance abuse and prevent diseases associated with tobacco use;
· specific advertising limitations and changes in corporate culture in the tobacco industry;
· payment of attorneys’ fees;
· establishment of a state enforcement fund with a one-time $50 million payment; and
· establishment of a nationwide advertising and education program to counter youth tobacco use and educate consumers about tobacco related diseases.
Although the agreement suggests areas for investment by the states, there is broad discretion in the manner in which jurisdictions may use settlement funds.
California is expected to receive payments totaling $21 billion over the next 25 years, half of which will go to the state, and half to local governments. Ten percent of the designated local government payments will go to the four litigating cities (San Francisco, Los Angeles, San Jose and San Diego). The remaining ninety percent of the local agency portion will be divided among county agencies based on the size of the population using the most recent census data, in this case the 1990 Census.
Approximately 26.8 percent of the local agency portion will be allocated to Los Angeles County. This comprises approximately 13.4 percent of the total funds allocated to California. The state has received initial 1998 and 2000 initial payments totaling approximately $588,677,000. Los Angeles County will receive an average of approximately $105 million annually. Los Angeles County received the initial payment of approximately $79.3 million on February 4, 2000, reflecting the initial 1998/1999 payment and a portion of the 2000 amount.
During the first year, due to initial start-up and 1998/1999 payments, it is estimated that as much as $30 million would be available for one-time-only funding for a variety of Board priorities. Currently $135 million has been received for 1998/1999 and 2000 periods for application to the $105 million proposed spending plan. It is proposed that $10 million be reserve for 2001, during which a $95 million payment is anticipated. The remaining $20 million will be available for one-time-only use. In addition, due to first year start-up, as much as $10 million may remain unexpended. Funds from these two sources will total $30 million for one-time-only funding for a variety of Board priorities.
The state’s allocation of potential recovery of settlement funds is anticipated to change over time with Los Angeles County’s portion being distributed as indicated below.
Los Angeles County Share of Tobacco Settlement Funds 1998-2025 (Estimated) | ||||||||
Year |
1998/1999 |
2000 |
2001 |
2002 |
2003 |
2004-07 |
2008-17 |
2018-25 |
$ in millions |
78.894 |
56.452 |
95.610 |
114.991 |
114.991 |
103.362 |
97.656 |
118.120 |
This schedule is based on the 1990 Census; with allocations subject to adjustments based on decennial census data and tobacco industry changes as discussed in Appendix One. No change in the schedule is expected before results of the Year 2000 census, no earlier than 2001. A relevant change in other County revenue is an anticipated reduction in funds for Los Angeles County earmarked for tobacco control under Proposition 99. Appendix Two describes these anticipated reductions.
Board of Supervisors Action
Unlike other jurisdictions, the Los Angeles County Board of Supervisors unanimously voted to use settlement funds to improve health and health care within the County. On December 1, 1998, the Board instructed the Auditor Controller to establish a separate General Fund designation for the Department of Health Services (DHS) to be designated the Tobacco Settlement Account, to receive Settlement funds. The Board further instructed DHS to develop a recommended spending plan for these funds, with priority given to the expansion of outpatient services, indigent health care, treatment of tobacco related diseases and the expansion of tobacco education and prevention programs.
This plan is an important building block to realize the vision for a healthier Los Angeles, one offering each person the opportunity to realize their health and economic potential. A major means to achieving this vision is each individual receiving timely, high quality prevention, diagnostic and treatment services throughout their life span. Further, realizing this vision requires that public agencies and partners work together to forge healthier communities and supportive social and physical environments.
Both prevention and treatment services are needed to improve the overall health of Los Angeles County residents. Thus, the vision is to improve the cost-effectiveness of our health investments through a combination of enhanced investment in cost-effective prevention, incremental expansion of services, and further strengthening of the safety net. However, even with these funds, the large and growing underserved population will still have unmeet needs absent significant state and/or Federal health system reform.
The Master Tobacco Settlement Agreement is an opportunity for Los Angeles County to realize broad goals consistent with the recently announced priorities by the Surgeon General to improve the health of the nation.1 These include:
· Increasing the span of healthy life for LA County residents by reducing the burden of chronic diseases and injuries;
· Reducing health disparities among various population groups and improving the distribution of available resources between geographic areas;
· Improving access to preventive services provided by the Department and its partners, that can, over time, reduce inappropriate demands on the safety net system; and
· Monitoring and evaluating the effectiveness and cost-effectiveness of the proposed investments.
The following plan proposes to reduce disease burden and resulting health expenditures by implementing interventions and strategies that will enhance prevention activities and improve early diagnosis and treatment of conditions accounting for a significant proportion of death and disability among Los Angeles County residents.
This report presents a 10-year plan of action that provides a balanced portfolio of investments in prevention, early diagnosis and treatment, expanded health care services and improved infrastructure to support the core mission of DHS. Recommendations are based on an extensive analysis of a) current health status, b) funds available to address major health concerns and Board priorities, c) major gaps in disease prevention, health promotion, and health care services, d) proven, cost-effective strategies and programs for addressing the major health problems, and e) opportunities to leverage Tobacco Settlement Funds.
This plan includes the following sections:
· Major health risks and serious health conditions impacting health in LA County.
· The major investment opportunities for addressing the serious health risks and conditions: (1) Prevention of Health Risks and Serious Conditions; (2) Early Diagnosis and Treatment of Remediable Health Problems; (3) Enhancing Open Door/Safety Net Systems; and (4) Strengthening Capacity and Improving Health Protection Systems.
· The proposed Implementation Plan.
Major Health Risks and Serious Health Conditions
The majority of the burden of disease for Los Angeles County residents results from preventable conditions, most of them chronic, including heart disease, cancers, stroke, diabetes, cirrhosis, and lung diseases such as emphysema1. Non-communicable diseases account for 82 percent of the total burden of disease to adult men in Los Angeles County, and for 69 percent in adult women. In 1997, chronic diseases accounted for over 61,000 deaths and more than 300,000 years of potential life lost among Los Angeles County residents.1
There is a large body of scientific evidence indicating that these conditions are preventable to a substantial degree. In Los Angeles County one-third of adult deaths is attributable to tobacco use, unhealthy diet, and lack of physical activity. The addition of other lifestyle-related exposures including heavy alcohol use, firearm related violence, risky sexual behaviors, illicit drug use, and unsafe driving leads to the conclusion that about one of every two deaths in Los Angeles County is attributable to preventable conditions. Studies throughout the country confirm that a substantial portion of hospitalizations is due to the effects of these risk factors- whether from trauma, cardiovascular disease, cirrhosis, cancer, or the effects of alcohol and other drugs.
Many of the conditions caused by tobacco use, such as heart disease and stroke, reflect a combination of risk factors, including poor nutrition, inadequate physical activity and inadequate screening and treatment for high blood lipids and high blood pressure. Alcohol use is a common denominator for many preventable diseases and injuries, from sexually transmitted diseases, including HIV, to unplanned teenage pregnancies, use of handguns to commit violence and motor vehicle and other unintentional injuries. Risk factors do not occur independently in vulnerable populations. They are clustered, particularly during adolescence when health related behaviors become well established. The table below provides a listing of the major health risks and associated chronic conditions.
For many conditions, successful prevention and control, both short and long term, require combining a variety of approaches to reduce known risk factors. Also, addressing a set of several risk factors can sometimes be more effective and more cost-effective than developing a separate prevention plan to address each risk factor.
Public health restructuring has laid a foundation for implementing a comprehensive set of chronic disease prevention and control programs. Beginning in 1998, reinvigoration activities have increased the Department's capacity in health promotion, chronic disease prevention and health assessment and epidemiology. Area health officers have been appointed to work with partners and community based organizations to implement programs responsive to community needs. Settlement funds provide an opportunity to build upon this foundation by investing in community based prevention activities, early diagnosis and treatment strategies and enhancing safety net and health protection systems.
Multiple Pathways: Health Behaviors and Health Outcomes.1
|
Major Health Outcomes |
Health Behaviorsa | |||||||
|
Smoking |
Lack of Physical Activity |
Poor Nutrition |
Intermediate Factorsb |
Alcohol Use |
Gun Ownership |
Unprotected Sex | ||
|
Hypertension |
Overweight |
|||||||
|
Heart Disease |
||||||||
|
Cancer |
||||||||
|
Diabetes |
||||||||
|
Stroke |
||||||||
|
Liver Disease |
||||||||
|
Arthritis |
||||||||
|
HIV/AIDS |
||||||||
|
Emphysema |
||||||||
|
Homicide/ Violence |
||||||||
|
Suicide |
||||||||
|
Unintentional Injury |
||||||||
a Health Behaviors represent health risk associated with the major health outcomes.
| ||||||||
Major Gaps in A Comprehensive Health Improvement Strategy for Los Angeles County
Preventing disease, promoting health and assuring necessary care to the nearly 10 million residents are critical responsibilities of County government and its many partners. The Department of Health Services contributes to these responsibilities by:
· Forging effective partnerships to protect and improve the health of County residents;
· Assessing the health of the population, assuring the general health and safety of the public, and developing and recommending policies to prevent disease and improve health;
· Targeting direct services toward the most vulnerable populations and ensuring a safety net for those that do not have other access to health care.
The Department’s success in fulfilling this mission is limited by inadequate funding and restrictions on the use of funds from the State and Federal Governments that affect its ability to choose the wisest strategies for improving health of vulnerable groups and the overall population. The challenge and opportunity afforded by the Master Tobacco Settlement is to select program and service priorities that transcend these barriers and maximize long-term benefits. The Department considered existing priorities that could potentially be addressed with additional revenue. These included both infrastructure and service expansion projects, which alone could exhaust the Tobacco Settlement funds. While not minimizing the need for revenue to support these projects, this plan seeks to make a significant step towards a balanced approach addressing both existing needs, as well as recommending investments to reduce the burden of disease among county residents.
Great care has been taken in the development of this plan to consider alternative options and opportunities as part of a comprehensive long-term strategy for community health improvement. An analysis was conducted identifying gaps in services and programs for specific populations and potential new funding streams to address these gaps. A more detailed discussion is included in Appendix Three. It is important to note, however, that Tobacco Settlement funds have been targeted for areas where funding is not available and revenue can be maximized. For example,
· Proposition 10 funds were identified as a funding stream to address existing gaps in services/programs for young children. Thus, the recommendations in this plan do not place high priority on interventions for this specific population.
· Similarly, Long-Term Self-Sufficiency funds are assumed to address service/program gaps for older children and teens.
· The proposed 1115 Waiver extension and its related amendments are assumed to be approved by HCFA without major revisions. Thus, the Healthy Students Partnership is expected to address the needs of school-age children and youth. Also, it is assumed that federal matching funds will be available to increase health access to low-income uninsured.
· The amounts targeted for ambulatory care enhancement, disease management, and some early diagnosis/treatment and infrastructure development would qualify for federal matching funds. The total precise amounts available would depend on the negotiated terms and conditions of the 1115 Waiver extension.
The Department will work with the Proposition 10 Children and Families First Commission and DPSS to continue to emphasize the needs, priorities and opportunities for intervention to positively impact the health of children and their families. In the event that these funding streams do not address these populations, we will re-evaluate our recommendations. The plan also assumes that the 1115 Waiver extension, as currently proposed, will be approved. It is estimated that $60 million of the proposed spending of tobacco settlement funds will be invested directly on the 1115 Waiver objectives currently under consideration by HCFA (See Executive Summary, Table One). In the event of significant reductions in anticipated revenue, priorities for the use of the Tobacco Settlement funds would be re-examined.
Health Improvement Opportunities
A balanced investment plan includes funding for prevention, early identification and treatment of health problems, expanded health services and improvements in infrastructure to support the core mission of the Department. Four categories of health improvement opportunities have been identified that are consistent with the Board direction, are faithful to the rationale underlying the Tobacco Settlement Agreement, and address the needs to substantially invest in prevention of conditions that adversely impact the health of large numbers of County residents:
· Prevention of serious health risks and health conditions,
· Early diagnosis and treatment of remediable health problems,
· Enhancing open door/safety net systems, and
· Infrastructure development and capital improvements.
It is recommended that the County invest a portion of the Master Tobacco Settlement Funds to reduce the preventable burden of disease and injuries in our population. As a part of this balanced portfolio, it is further recommended that a significant portion be invested to strengthen the safety net and build capacity. Strategies and interventions will be proposed corresponding to these four areas of investment that will help fulfill the Department’s core functions.
Goals of the Proposed Plan
The broad mission underlying the recommended allocation of Tobacco Settlement funds is to reduce disease and improve health among Los Angeles County residents. The specific goals of the proposed activities in this plan are to:
· decrease tobacco use,
· increase behaviors that promote health and chronic disease, specifically increase physical activity and improve nutritional behavior,
· increase recognition and appropriate treatment of depression, excessive alcohol use and substance abuse,
· reduce risk taking behavior among adolescents,
· increase the amount and quality of prevention services delivered in ambulatory care settings,
· decrease preventable hospitalizations,
· increase health outcomes for those with chronic diseases,
· improve disease surveillance and evaluation, and
· improve accountability for measurable outcomes.
The table below presents a matrix of the proposed plan goals and their relationship to the four health improvement opportunities described previously. A wide variety of carefully crafted interventions designed to reduce risk and promote healthy behaviors have either been evaluated to be effective or considered to have significant population benefit. It is recommended that priority be given to approaches for which effectiveness is established but to also invest in promising approaches in conjunction with careful evaluation. Consistent with a comprehensive approach, interventions in more than one area may be combined to address a single goal. It is further proposed that the County undertake these investments in full partnership with other public agencies and private community organizations.
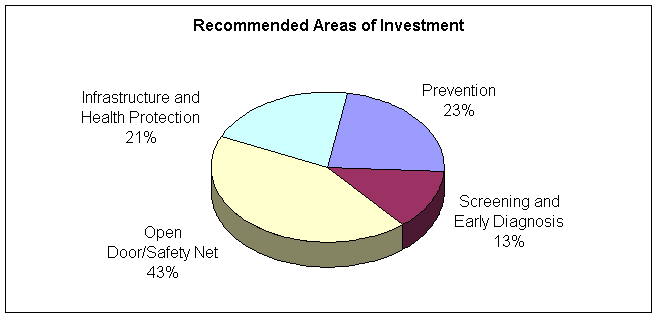
The figure below shows the division of recommended funding into four major areas of investment. Two critical areas are prevention and early diagnosis and screening activities to reduce the burden of chronic disease and serious health problems among Los Angeles County residents. The focus on preventive care in clinical settings is exemplified by the recent implementation of the Office of Women’s Health Cervical Cancer Screening Initiative. This successful set of activities demonstrates how the translation of policy decisions and priorities into programs emphasizing screening, early identification and treatment can help reduce diseases disproportionately impacting sections of our population.

Significant investment is also recommended to enhance the safety net system to improve access to health services. While a variety of providers (private hospitals, emergency rooms, etc.) contribute to the “safety net” of emergency services available to Los Angeles County residents, DHS and its partners provide access to a full range of services, expanding the role of safety net to a broader array of preventive and early diagnostic and treatment services. As "open door providers," DHS and its public/private blended network are moving towards an emphasis on prevention that can ultimately reduce the burden of disease on the population and the public health care system. The proposed plan will greatly advance this transformation by focusing on vulnerable populations through selective interventions and strategies.
Investments are also proposed to increase the Department's health protection capacity and to improve infrastructure. The LA Health Survey is an example of the benefits of investments to improve the Department’s capacity to assess and monitor health related issues in Los Angeles County. These comprehensive surveys of County residents provide information about health needs, health care access issues and opportunities for intervention for use by the Department, its partners, and community stakeholders to plan and implement strategies to improve health and increase access in each part of the County. The LA Health Survey data has been particularly important in demonstrating the need for extension of the 1115 Waiver.
Overview of Strategies and Interventions
This section presents interventions corresponding to the four areas of health improvement opportunity. Associated with these areas of investment are themes that run consistently throughout the proposed interventions: 1) tobacco control activities, 2) disease prevention and health promotion efforts aimed at reducing health disparities among Los Angeles County women, and 3) a focus on clinical service enhancement and increased capacity.
A variety of tobacco control interventions are woven throughout the plan. The genesis of the settlement and that tobacco use remains the greatest preventable cause of death in Los Angeles County are strong reasons to allocate a significant portion of this investment to reducing tobacco use through prevention and cessation and reducing the toll of tobacco related diseases through improved case finding and disease management for the medically underserved population.1 Further, there is strong evidence that sustained significant investment in tobacco control can reduce tobacco use. Appendix Four provides a detailed discussion of the large benefits a comprehensive tobacco control program can return for the health of Los Angeles County residents.
Integral to the proposed interventions are disease prevention and health promotion efforts that address diseases that constitute the majority of death, illness, and disability among Los Angeles County women. These include: heart disease, breast and lung cancer, alcohol dependence, stroke, diabetes, depression, and arthritis. Promoting healthy food preparation and selection, physical activity for the sedentary and overweight, incorporating skill-building and social support, de-stigmatizating help-seeking behavior, and other health promotion efforts integrated in the ambulatory care context can have significant positive effects on women’s health
The proposed plan also includes interventions focusing on clinical service enhancement, building on efforts to provide a seamless system of care while reducing disparities in access. Further, it contains a proposal for significant investment in infrastructure development, i.e., improving key elements of our health system capacity – MIS, surveillance and quality assurance activities – to enable us to better understand and plan for health needs, and monitor and evaluate our performance.
These themes and the proposed interventions are consistent with the Board directive and the intent of the Tobacco Settlement. Further, the investments outlined in this plan are consistent with the restructuring of the department under the 1115 Waiver. The plan recommends further enhancement of ambulatory care by allocating significant annual amounts towards meeting the local match requirements to meet annual visit targets, and investing in information system infrastructure, disease management and programs that reduce the burden of disease on specific populations that relying on the open door/safety net delivery system.
The table below provides an overview of the proposed interventions, categorized by the four health improvement opportunities (prevention, early diagnosis and treatment, safety net enhancements, and improving capacity and infrastructure). As illustrated, each intervention involves multiple approaches, ranging from support for community based interventions, to tobacco prevention and control, to building capacity and infrastructure.
To determine the return on investments, each intervention will include impact/outcome and performance measures. Programs developed based on this plan would be required to include procedures for systematic monitoring and evaluation to assure that they are effective in producing the desired, measurable outcomes. A proportion of funds (between one and five percent depending on the complexity of the program and the required evaluation) will be provided for internal and/or external evaluations. In addition, ten percent of the funding for interventions in the areas of prevention, early diagnosis and treatment, capacity building and health protection will be held in reserve to address potential changes in priorities and serve as a buffer against future funding reductions.
Overview of Interventions
| |||||
|
INTERVENTIONS, CATEGORIZED BY AREAS OF OPPORTUNITY FOR IMPROVEMENT (Proposed allocations assume $105 million annually.) |
Prevention in Clinical Care Delivery |
Tobacco Prevention And Control |
Chronic Disease Prevention |
Capacity & Infrastructure |
Recommended Spending Allocation
|
PREVENTION (23 percent) |
|||||
· Promoting Healthy Behaviors ($13 M) |
X |
X |
12% | ||
· Mobilizing Communities for Health ($2 M) |
X |
X |
2% | ||
· Reducing Tobacco Use ($5 M) |
X |
X |
5% | ||
· Promoting Physical Activity Among Seniors ($4 M) |
X |
4% | |||
EARLY DIAGNOSIS AND TREATMENT OF REMEDIABLE PROBLEMS (13 percent) |
|||||
· Smoking Cessation ($7 M) |
X |
X |
X |
6% | |
· Alcohol/Drug Use and Depression Screening and Treatment ($4 M) |
X |
X |
4% | ||
· STD Prevention, Screening and Treatment ($3 M) |
X |
3% | |||
ENHANCING OPEN DOOR/SAFETY NET SYSTEMS (43 percent) |
|||||
· Ambulatory Care Enhancement ($40 M) |
X |
X |
X |
38% | |
· Cost Effective Management of Diseases and Conditions ($5 M) |
X |
X |
X |
5% | |
STRENGTHEN CAPACITY AND IMPROVE HEALTH PROTECTION (21 percent) |
|||||
· Infrastructure Development ($10 M) |
X |
10% | |||
· Capital Improvements ($12 M) |
X |
11% | |||
TOTAL FUNDS |
100% | ||||
Using an estimate of $105 million per year, the proposed plan includes significant investments in interventions addressing tobacco control, chronic disease management, and chronic disease prevention and control. Tobacco use prevention and control activities are represented in both prevention and early diagnosis and treatment interventions and are estimated to represent an investment of approximately 15 percent of total settlement funds. Appendix Five compares proposed investments in tobacco control with the Centers for Disease Control and Prevention recommendations for comprehensive tobacco control programs. Like the CDC plan, the proposed Los Angeles County plan emphasizes tobacco control and prevention and treatment of chronic disease.
In the following section, interventions corresponding to the four areas of health improvement opportunity are presented. Each intervention proposed has been recommended for inclusion based on demonstrated effectiveness and recommended best practice.1,1,1,1,1,1,1,1,1 Appendix Six summarizes the literature and programs reviewed to inform the development of the recommended interventions.
Four proposed interventions are designed to reduce the risks associated with chronic diseases and promote healthier behaviors among County residents. The table below provides the approximate proportion of funds that would be allocated to each of these broad county-level interventions.
Suggested Prevention Interventions | ||
Focus of Interventions |
Target Population |
Suggested Funding |
Promoting Healthy Behaviors |
Adults in Underserved Areas |
$13 million |
Mobilizing Communities for Health |
General Population |
$2 million |
Reducing Tobacco Use |
General Population |
$5 million |
Promoting Physical Activity Among Seniors |
Seniors |
$4 million |
Total Community-Based Prevention Interventions |
$24 million | |
· Promoting Healthy Behaviors: Community Based Nutrition and Physical Activity, Smoking Cessation and Violence Prevention Interventions
Smoking and physical inactivity are demonstrated to increase risk for common preventable illnesses.1 A significant proportion of mortality among adults is related to the use of tobacco, unhealthy diet, and lack of physical activity.1 The goal of interventions in this category is to increase resilient behaviors (fruit/vegetable consumption, exercise) and reduce risk behaviors (smoking, violence) among adults in underserved areas of the County with an underlying mission of reducing health disparities.1,1,1,1,1,1 Interventions in this category include:
· Providing training programs culturally tailored to empower communities to integrate physical activity and healthy nutrition into their daily lives.
· Developing a targeted media campaign in concert with Service Planning Areas and local voluntary agencies to promote community programs, healthy nutrition and home-based physical activity opportunities.
· Developing gender-specific violence prevention programs in underserved communities targeting young adults (aged 18-25) to improve vocational skills/readiness, parenting skills, and family planning.1
· Delivering free fitness instruction/nutrition education and smoking prevention and cessation activities in a variety of sites in underserved communities including existing DHS clinical and public health sites, DHS contractor community-based organizations, PPPs and Healthy Student Partnership schools.1,1
· Supporting efforts to develop worksite wellness programs within underserved communities, with a special emphasis on small businesses.
The anticipated outcomes of these interventions over five years are: (1) increase in physical activity levels by 5 percent; (2) in combination with other interventions, a decrease in smoking by 2.5 percent; and (3) increase in daily servings of fruits and vegetables by 1 serving.
· Mobilizing Communities for Health
Interventions recommended to mobilize communities around policies that significantly influence health would target the general population and provide support for programs with demonstrated effectiveness. Building on successful strategies used in Los Angeles County and other jurisdictions,1,1,1,1 the overall goal of interventions in this category is to increase the effectiveness of community based agencies, coalitions and partnerships in addressing tobacco, drug and alcohol use, healthy nutrition and youth physical inactivity.1 Comprehensive community based interventions must include activities to address barriers to risk reduction to assure effectiveness. Programs supported in this category are also expected to include monitoring and evaluation activities to assure program quality and effectiveness. Examples of interventions in this area include:
· Funding programs with demonstrated effectiveness that mobilize communities to work for change in the areas of tobacco, alcohol/drug and violence prevention and physical education promotion in public schools.
· Providing one-time funding to support enforcement of tobacco control laws and regulations related to the advertising, sale and use of alcohol and firearms in the County and to work more effectively with cities within the County to implement similar regulations.
· Assisting communities to adopt effective prevention activities, e.g., increasing availability of fresh produce in grocery stores.
· Forming a Community Health Assessment Rapid Response Team (CHARRT) to conduct household health surveys of community residents and to assist community health improvement groups.
Anticipated outcomes of these community based interventions over five years include: (1) in combination with other interventions, a 2.5 percent decrease in smoking; (2) decrease in sales of tobacco, alcohol and firearms: and (3) acquisition and use of better community level data on health risks.
The goal of these interventions is to increase community capacity to develop effective, tobacco prevention and health promotion programs. Examples of interventions in this category include:
· Implementing gender, ethnic, and age appropriate tobacco-use prevention and education campaigns combining messages on tobacco prevention, cessation and protection from second-hand smoke.
· Supporting grassroots promotion activities, local media campaigns, event sponsorship and other community partnerships to support and reinforce existing tobacco statewide campaigns.
· Assisting community based organizations within Service Planning Areas to facilitate the planning, implementation and evaluation of their prevention programs.
Anticipated outcomes of these interventions over five years include: (1) decrease in cigarette smoking prevalence among youth aged 12 to 17 years by 2.5 percent; and (2) decrease in in-home environmental tobacco smoke exposure of adults by 10 percent.
Exercise studies targeting seniors have demonstrated improvements in mental ability, mood, strength, and agility associated with decrease in falls, extended independent living and an overall higher quality of life. Anticipated program outcomes include: (1) significant improvement in mental ability, mood, strength and agility among seniors; and (2) significant decreases in falls, extended independent living, and overall higher quality of life among seniors.
Recommended community based prevention and health promotion interventions are a foundation for efforts promoting individual behavior change. In addition to implementing broad prevention programs to reduce the likelihood that health conditions develop, effective programs are needed to diagnose emerging health problems early and assure appropriate treatment to prevent more serious disease and complications.
Strategy 2. Early Diagnosis and Treatment of Remediable Problems
Countywide, chronic diseases account for the majority of death and disability. Poor and uninsured clients have higher than average rates of most chronic diseases and are more often victims of violence. 1 A significant proportion of care for the uninsured and the poorest segment of our population is provided by DHS and its Public Private Partners (PPPs). Consequently, focusing on enhancing the quantity and quality of early diagnosis and treatment of remediable health conditions in these settings will have a significant impact on the health disparities observed among different groups within the County. In addition, working in collaboration with professional medical, nursing and other organizations at the County level can improve recognition, counseling and early treatment for the broader population of our residents. Three strategies are recommended to enhance early diagnosis and treatment of health problems:
Suggested Early-Diagnosis and Treatment Interventions | ||
Focus of Interventions |
Target Population |
Suggested Funding |
Tobacco use screening and counseling |
Primary care patients |
$7 million |
Screening and treatment for substance abuse and depression |
Primary care patients |
$4 million |
Screening and treatment of STDs |
High Risk Adolescents |
$3 million |
Total Clinic-Based Prevention Interventions |
$14 million | |
Screening and follow-up activities are an essential part of routine care and are typically well integrated into health care providers’ mission, priorities and resources. However, there remain important opportunities to expand these services, with particular attention to quality control and the strong linkage between screening and follow-up. The following areas are recommended for additional funding from Tobacco Settlement Funds.
· Screening for tobacco use and counseling using established guidelines for physicians and other health professionals
We estimate that 170,000 smokers use County-funded health care services.1 In Los Angeles County, an estimated $1 billion per year in direct medical expenditures is attributable to tobacco use. One strategy for reducing these avoidable costs is physician screening and counseling. Brief advice to quit from a physician or other health care professional produces small, but consistent, increases in cessation (3 to 5 percent) after one year.1,1 Thus, the cumulative effect of this intervention over time will contribute greatly to a reduction in tobacco related health care costs. The goals of this screening and counseling intervention over five years are to:
· Identify and screen 90 percent of smokers seen by open door providers.
· Provide cessation counseling to 50 percent of smokers seen by open door providers.
· Decrease smoking prevalence by 4 percent.
· Alcohol/drug use and depression screening, counseling, treatment and appropriate referral as part of primary care
Individuals with substance abuse problems and depression utilize health care services at higher rates than do others.1 This investment would increase the number of patients in DHS and private partner sites who are screened, counseled, treated and appropriately referred for drug and excessive alcohol use in primary care settings. Most physicians are not aware of depression prevalence or clinical treatment guidelines, and do not routinely screen for depression. There are many good treatments available, making many costs associated with depression avoidable. This intervention would establish a pilot program to examine the effectiveness of depression screening and treatment in selected primary care sites.
Approximately 1.2 million adults and children suffer impairment due to substance abuse and we estimate that 351,000 of these receive County-funded health care services. We estimate that about 20 percent of the 175,000 “heavy utilizers” of the County system are depressed (35,000 people). The goals of this screening and treatment intervention are to:
· Increase the number of patients appropriately screened and treated for depression at DHS and PPP sites by 20 percent.
· Decrease utilization of County-funded health services among depressed patients by 10 percent.
· Increase the number of patients with substance abuse problems who are counseled by 20 percent.
· Decrease utilization of County-funded health services among patients with substance abuse problems who were screened and counseled by 10 percent.
· Decrease in number of episodes of driving under the influence (DUIs), domestic violence, and emergency room injury-related visits among those screened and counseled.
· Screening for STDs (including HIV screening) and related treatment in high-risk populations, such as adolescents in juvenile detention facilities.
There are high rates of chlamydia and gonorrhea in teens, especially incarcerated youth, many of whom rely on County-funded health care services. Untreated chlamydia results in serious and costly reproductive health consequences for women, including pelvic inflammatory disease, infertility, and ectopic pregnancies that can lead to maternal deaths. About 90 percent of chlamydia-infected teens do not have symptoms and therefore do not seek care. In addition, untreated STDs increase the risk for HIV infection.
It is estimated that cost savings from this intervention will offset County expenditures treating pelvic inflammatory disease, ectopic pregnancy, epididymitis, and new chlamydia and gonorrhea infections. Screening and treatment of female and male adolescents can avert all of these conditions. There are numerous other health outcomes that would be averted by this intervention, including infertility, pre-term births, and neonatal illnesses.1,1 Overall, it is estimated that the cost savings from screening and treating chlamydia and gonorrhea among teens in juvenile detention facilities will result in $1.7 million costs savings to DHS.1 The goals of this screening and counseling intervention are to:
· Screen 90 percent of juvenile detainees for chlamydia, gonorrhea and HIV (approximately 29,000 teens).
· Provide treatment to infected teens (approximately 4,400 teens).
· Decrease prevalence of chlamydia and gonorrhea among juvenile detainees by 5 percent.
· Expand screening and treatment of chlamydia and gonorrhea to all County ambulatory care sites providing family planning services.
The open door/safety net system in Los Angeles County, even with recent expansion in ambulatory care, is vulnerable given the needs of the large and rising uninsured and underinsured populations. Los Angeles County’s application to extend the 1115 Waiver proposes a stronger focus on increased prevention; improving disease management and a further increase in ambulatory care capacity. Ambulatory care services are a central link in prevention activities. Expanding access to services is the first step. Expanding the scope of these vital services to incorporate an increased emphasis on prevention and early detection of serious health problems increases the benefit derived from quality primary care.
Tobacco Settlement funds, because they provide a large revenue stream, can be used to strengthen the ambulatory care delivery system and maximize total available funds under the 1115 Waiver, providing an open door/safety net system emphasizing cost-effective, preventive care, early diagnosis and disease management for all patients.
To maximize service availability, DHS is developing an innovative program for increasing the clinical quality, patient satisfaction and cost-efficiency of clinical services. The Clinical Resource Management program (CRM) is a structured methodology that results in patient, family, or provider behavior change affecting the risk of acquisition, natural history, treatment, or cost of health and sick care.1 There are three inter-related components to the CRM program: Inpatient Clinical Pathways, Comprehensive Disease Management, and Case Management.
Suggested Safety Net Enhancements | ||
Focus of Program |
Target Population |
Suggested Funding |
Ambulatory Care Enhancement |
$40 million | |
Cost Effective Management of Diseases and Conditions |
$ 5 million | |
· Inpatient Clinical Pathways |
Selected DHS inpatients |
|
· Comprehensive Disease Management |
Patients who are appropriate for the six disease management protocols |
|
· Case Management |
High utilizers |
|
Total Clinical Resource Management Programs |
$45 million | |
· Ambulatory Care Enhancement
To further increase access to ambulatory care and enhance the mix of services through cost-effective methods that serve uninsured patients relying on both DHS and PPPs, it is recommended that we program an average of $40 million per year. The funds would assist us in delivering additional primary and specialty care services in outpatient settings through both PPPs and DHS-operated facilities – and assist in leveraging local funds with additional federal funding.
Ambulatory care enhancement funds should not be used solely to increase visits, but to optimize clinical functions with opportunities to further infuse public health principles into the delivery of services. This means that funds should be targeted to screen for high burden conditions (such as substance abuse and depression), encourage health promotion and disease prevention during the clinical encounter, and enhance population-based quality improvement functions. Thus, it is proposed that Tobacco Settlement funds for ambulatory care enhancement be focused on:
· meeting the proposed 1115 Waiver-related ambulatory care commitments currently under consideration by HCFA;
· integrating public health services as part of basic primary care services in ambulatory settings;
· creating financial incentives for ambulatory care providers to meet a full range of established, age-appropriate screening and assessment prevention guidelines; and
· enhancing the evaluation and monitoring of the quality of care for high burden conditions.
· Cost Effective Management of Disease and Conditions
Clinical pathways focus on County DHS’ top diagnostic-related groups (DRGs) providing structured physician order sets and documentation tools that will reduce expenditures by reducing variability between physician practices in managing homogenous groups of patients. It is expected that inappropriate variation and care, both in terms of length of stay and therapeutic choices, will be reduced dramatically. Reducing unnecessary variations in care will result in operational efficiencies, improved outcomes, improved provider efficiency and timeliness of service delivery, and reduced numbers of inappropriate re-admissions.1 The supporting record-keeping and information system will facilitate the collection of best practice data and measurement of clinical outcomes as a by-product of care. Funds will be used for hiring supplementary professional and support staff, effective forms management, and data collection and analysis.
Consistent with a prime 1115 Waiver goal, the purpose of the comprehensive disease management component of CRM is to focus on specific chronic diseases to reduce inappropriate inpatient and emergency room utilization. It is the outpatient corollary of clinical pathways. The disease management protocols represent an integrated approach to manage the complete spectrum of disease, from diagnosis to outcome. Full implementation of these disease management programs will be the first time that a large integrated, multicultural, multilingual public health system is attempting to implement such a profound change in clinical practices.1
Patients seen in DHS facilities and PPPs have high rates of chronic conditions whose outcomes, measured in health, quality of life and mortality, improve with proper management. DHS has already developed four disease management protocols and will finalize two more by 2005; HIV/AIDS, adult diabetes, congestive heart failure, pediatric asthma, hypertension (pending), and co-occurring mental health conditions (pending). Four of these diseases are smoking related or impacted by tobacco exposure.
Funds will be used for education of providers and patients, hiring of supplementary professional and support staff to assure appropriate counseling, continuity of care, and record-keeping while expanding the number of individual patients served.
The case management component of CRM is designed to manage the care of individuals who are “high utilizers” of the DHS/PPP system. These case management services will coordinate clinical care across providers for patients with multiple and complex medical conditions to provide more efficient and effective care. Because these individuals have multiple diseases or conditions, their care is not specifically impacted by the Inpatient Clinical Pathways or Disease Management programs that are disease- or condition-specific. The case management services will include assessment, planning, implementing, coordinating, and evaluating options and services for the patient. Funding requirements are similar to those of the disease management program.
The estimated funds needed for full implementation of clinical resource management interventions do not reflect potential revenue losses. Our efforts to reduce inpatient services may have negative revenue consequences. The degree of revenue losses is dependent on our success in obtaining a 1115 Waiver amendment that addresses the current economic disincentive associated with efforts to reduce inpatient utilization through improved inpatient clinical efficiencies and disease management.
Constraints in the system's ability to provide comprehensive services and programs to improve, promote and protect health extend beyond service availability. In some instances the constraints are physical—outmoded or insufficient capacity of facilities—while in others, they are limitations in operating budgets to expand needed services. Further, there are significant internal barriers to comprehensive continuous care to effectively manage special populations, such as deficient tracking and information systems across the delivery system, particularly between DHS and its partners.
The Department is charged also with a range of health protection activities designed to safeguard the health all county residents. Improved disease and health risk surveillance of populations is another critical necessity to better estimate need, define priorities for personal health care and public health services, and to increase system accountability through improved monitoring and evaluation of how well DHS and partners are meeting our collective goals.
It is recommended that $22 million per year be invested in two priority areas: Infrastructure Development and Capital Improvements.
Capacity and Health Protection System Improvements | |
Focus of Program |
Suggested Funding |
Infrastructure Development |
$10 million |
Capital Improvement |
$12 million |
Total Infrastructure and Capital Improvements |
$22 million |
· Infrastructure Development
To promote systems integration across the delivery system and empower clinicians, planners, administrators, epidemiologists and others to directly manage, monitor, evaluate, and report on patient care and population health status, it is recommended we invest $10 million additional funds in information system technology and training. Fifty percent of this amount would be invested in clinically based projects that improve clinical record keeping to track and evaluate patient care. The other 50 percent would be invested in population based systems for a data warehouse, web-based application to facilitate information exchange with county residents, health care providers and a wide range of public and private organizations, enhancement of disease surveillance, and other data projects to track progress in meeting health goals and increasing accountability. The specific projects to be supported with Tobacco Settlement funds include:
· the data warehouse project to link local data repositories to centralize collection of essential health care data and provide access to users across the delivery system;
· further development of web-based and web-enabled applications to facilitate exchange and dissemination of information;
· improvement in clinical information technology to track and evaluate patient care across the delivery system including, where feasible, the PPPs; and
· enhancement in the surveillance and assessment of diseases, health risk factors, disease prevention and health promotion efforts throughout the county to better monitor and evaluate system performance and accountability.
· Capital Improvements
To significantly upgrade and expand facility capacity for ambulatory care, it is recommended that $12 million per year be targeted for capital improvements. These funds would be used to guarantee repayment on capital construction, supporting approximately $150 million in capital spending based on the priorities in the Board- approved DHS capital plan that also considers the needs of the PPPs as part of the DHS system. Capital improvements could include building/refurbishing of physical facilities. Expected outcomes are more cost-effective, integrated delivery of health and other human services, and increased use of DHS and PPP facilities by patients with health benefits.
X. Implementation
The proposed ten-year Health Improvement Strategy is divided into three phases: planning, program implementation, and a mid-course review and adjustment. The Strategy consists of four initiatives: (1) Prevention, (2) Early Diagnosis and Treatment, (3) Enhancing Open Door/Safety Net Systems (including ambulatory care and clinical resource management), and (4) Strengthening Capacity and Improving Health Protection Systems.
Many of the proposed interventions in the Prevention and Open Door/Safety Net initiatives require a community-based planning process for the development of area-specific program recommendations. Allocation of resources will be based on unmet need formulas developed for each of these two initiatives. Examples of factors that may be considered for a Prevention allocation formula include population size, disease burden, the number of high-risk teens, disparities in health and health behaviors and poverty. Factors for the Open Door/Safety Net allocation formula include distribution of unmet need for ambulatory care services, self-reported levels of difficulty in obtaining medical care, and preventable hospitalizations for selected illnesses in public hospitals.
Upon final Board approval for the Open Door/Safety Net initiative, the Department will allocate designated funds to DHS facilities and initiate a formal process to identify new private partners or expand services of current providers. For the Prevention initiative, a competitive bid process will be used to solicit proposals from private agencies, as well as DHS facilities and programs, in an effort to identify the best public or private entities to provide services.
Other jurisdictions may be interested in securing Tobacco Settlement funds to address needs within their communities. In developing this plan, we examined the health needs of all County residents, thereby including the residents of the 88 cities within the County. Consequently, the interventions proposed will benefit city residents. We anticipate that some cities may wish to apply for funding when RFPs and other processes for allocation of funds are initiated.
Major steps in the planning process include:
· By June 20, 2000, submit report to Board of Supervisors.
· By July 31, 2000, develop resource allocation formulas for Prevention of Health Risks and Enhancement of the Open Door/Safety Net initiatives.
· By July 31, 2000, outline steps and timeline for community-based planning process for implementation of the Prevention and Open Door/Safety Net initiatives. The process will include participation of a central Planning Council and SPA-based community groups.
· The submission of final SPA-based plans and Countywide report to the Board of Supervisors for review and approval.
The program implementation stage will include the following major steps:
· Sixty days following Board approval, develop Requests for Proposals or other appropriate formal processes to determine the public and private providers who will implement the Prevention and Open Door/Safety Net initiatives.
· Ninety days following Board approval, implement the administrative, evaluation, quality assurance, and monitoring components necessary for each of the initiatives.
· Implementation of clinical resource management interventions will include the following steps: (a) implementation of four of the 39 clinical pathways each fiscal year; (b) pilot-test all six disease management protocols and implement protocols for pediatric asthma and coronary heart failure by January 2002, and HIV and diabetes by February 2003; and (c) by February 2003, implement all case management programs for high utilizers.
Two phases of reporting are envisioned following approval of this preliminary plan:
· Reporting during development of Implementation Plan: Following approval of this plan, detailed action plans will be developed for each set of investments. During this initial period a report will be submitted to the Board every 60 days detailing progress in developing action plans, interventions and processes to allocate funds both internally and externally. A detailed implementation plan will be prepared to describe program and intervention rollout.
· Reporting following development of Implementation Plan: Following completion of the implementation plan, quarterly reports on program and intervention progress will be submitted to the Board. Implementation progress reports will include descriptions of processes used to engage the communities and stakeholders in program planning and implementation and timelines, as well as results of competitive bid and other allocation processes. Progress reports will also include descriptions of methods developed to monitor program implementation, as well as periodic reports of program milestones. When appropriate both process and outcome measures will be reported, however it is anticipated that initial reports will be limited to process and intermediate outcome measures.
Intervention project reports will be required for all areas of investments. To ensure accountability performance measures will be established for each program and will be included in semi-annual progress reports along with current expenditures.
A mid-course review will be conducted to assess performance in achieving desired outcomes, identify and address unanticipated barriers and examine the accuracy of cost figures. A revised strategy will be developed and submitted to the Board for approval if indicated by this review.
Appendix Seven provides the detailed implementation plan detailing the major steps, timelines, and accountable groups or managers for implementing the 10-year health improvement strategy.
The process to obtain stakeholder input on this plan includes a series of stakeholder meetings, a written report of stakeholder comments, and presentation of the report to the Health Planning Council to obtain their advice and recommendations. Using the Department's extensive database of community stakeholders, organizations, providers and advocates, a series of Service Planning Area based meetings will be held. Input will also be gathered during upcoming meetings of stakeholder groups with Countywide representation and employee forums at DHS facilities. For consistency, all stakeholders will receive the same presentation, and will be asked to respond to a set of specific questions.
XI. Conclusion
The recommendations provide a balanced portfolio between a) more prevention, early diagnosis, counseling and follow-up, b) more cost-effective and supportive care for chronic illnesses c) expanded services, and d) improved infrastructure support. These recommendations would satisfy all or most of our funding requirements under the proposed Waiver extension, improve health and reduce disease burden through cost-effective prevention, and provide data and systems to improve responsiveness and accountability for both personal and public health functions. Impacts of the recommended plan should be reduced preventable illness straining the open door/safety net system, improved health status, reduced disparities in health and access to health care services, resulting in a healthier labor force and improved economic productivity for Los Angeles County.
APPENDIX ONE
Factors Impacting Tobacco Settlement Payments
In addition to changes in allocations to the states based on population changes, a number of other factors could potentially impact the amount of settlement funds available over the twenty-five year period of the agreement. These include:
· Actions of the federal government to seek a share of the funds to recover tobacco related Medicaid costs.
· The tobacco industry could reduce payments if nationwide sales drop with adjustments based on volume of cigarettes shipped within the United States.
· The 45 cents per pack cost increase imposed by the tobacco industry to support the settlement costs would also result in a reduction in sales.
· Successful lawsuits by local governments could impact the amount available for distribution within a state. Any future payments to local jurisdictions would be offset by the amount allocated to the particular state.
APPENDIX TWO
Status of Proposition 99 Funds
Although California and Los Angeles County have mounted significant efforts to reduce tobacco use through Proposition 99 funds, this is a decreasing revenue source. A significant decline in indigent care revenues funded by Proposition 99 is anticipated in FY 1999/2000. Based on the Governor’s proposed budget, funding in FY 1999/2000 is estimated to be about half of the amount received for the previous year, a loss of about $32 million in funds used to support health care services to indigent patients.
In Los Angeles County, reduction in Proposition 99 revenue results in a loss of funds available for tobacco control programs as indicated in Table Two below. In FY 1997/1998, Los Angeles County received a high of over $11.7 million in Proposition 99 funds, a per capita expenditure of $1.22 for each County resident. A 59 percent decrease in the Proposition 99 allocation in FY 1999/2000 resulted in the loss of almost $7 million, dropping per capita expenditure to $0.50 per county resident. Flat funding is anticipated for both the FY 2000/2001 and FY 2001/2002.
Los Angeles County Proposition 99 Tobacco Control Funds | ||||||
Proposition 99 $ |
Year | |||||
96/97 |
97/98 |
98/99 |
99/00 |
00/01 |
01/02 | |
Annual Allocation ($millions) |
$9.137 million |
$11. 771 million |
$6.183 million |
$4.786 million |
$4.786 million |
$4.786 million |
Per capita Expenditure
|
|
$1.22 |
$0.64 |
$0.50 |
$0.50 |
$0.50 |
In addition, as a result of continued declining tobacco consumption, recent manufacturer increases, and Proposition 10 tobacco taxes, tobacco sales are estimated to drop significantly this coming year. The State of California Legislative Analysts Office estimated that tobacco sales will decline between 17and 20 percent in FY 1999-2000.
APPENDIX THREE
Major Gaps in A Comprehensive Health Improvement Strategy for Los Angeles County
The following is an analysis of program/service areas that should be part of a comprehensive long-term strategy for community health improvement. For each area, there is a brief description of existing efforts and potential funding for addressing further expansion. The purpose of this matrix is to isolate areas where funding is not available and where discretionary
Master Tobacco Settlement funds can best be invested.
Analysis of Major Gaps
Health Area |
Status of Existing Programs |
Potential New Funding Streams to Address Gaps |
Recommend Gaps To Be Addressed Through Tobacco Settlement Funds |
By Vulnerable Population |
|||
Mothers and Young Children |
Perinatal care and prevention services for young children are available. Need for comprehensive approaches for ensuring optimal health and development of young children. |
Proposition 10 |
|
Older Children and Teens |
Preventive and screening services are available through CHDP and other programs. Treatment services for vision, hearing, dental and other conditions identified through CHDP screenings remain a major gap. There is a huge need to foster approaches addressing multiple risk behaviors that do not get funded through current categorical funding streams. |
Long-Term Self-Sufficiency Healthy Student Partnership |
|
Seniors |
Very limited categorical funding available for health assessments and regional elder abuse services. There are no other categorical or general funds available to address health promotion, and disease prevention and management for seniors. Access to health care is not as high a concern as with children and adults. |
None |
U |
U Health Area |
Status of Existing Programs |
Potential New Funding Streams to Address Gaps |
Recommended Gaps to Be Addressed through Tobacco Settlement Funds |
By Health Risks or Concern |
|||
AIDS, TB, and other infectious diseases |
Local, state, and federal categorical funds available. Improvements are needed in the core competencies of assessment and assurance. |
For some diseases and conditions, new categorical funding is available depending on disease trends |
|
Chronic Diseases/ Injury Prevention |
Very limited local and state funding available. Funding levels do not correspond with the level of disease burden. Funding needed for all facets of a comprehensive approach: disease and injury prevention, early diagnosis and treatment, and disease management. |
None |
U |
Substance Abuse |
Local, state, and federal funding available. Great potential to impact this area through routine screening by health practitioners. |
Long-Term Self-Sufficiency |
U |
Health Access for the Uninsured |
Local, state, and federal funds available. Funding levels do not correspond with the levels of burden. Capital project funds are needed to restore facilities to good condition and to add capacity in the system to deal with unmet service needs. |
1115 Waiver, requiring local match |
U |
Service Integration |
There are major opportunities to eliminate fragmentation and uncoordinated service delivery among primary care, Aspecialty@ public health, mental health, and substance abuse services. Major strategies include comprehensive screening by primary care practitioners, case management, and formalizing linkages. |
None |
U |
Breast and Cervical Cancer Screening |
Two state funded programs (BCCCP and BCEDP) provide funds for outreach and education to increase screening utilization among low-income women not eligible for MediCal/Medicare. |
None |
U |
APPENDIX FOUR
Rationale for Investment in Tobacco Control
The genesis of the settlement is strong reason to allocate a significant portion of this investment to: 1) reduce tobacco use through prevention and cessation, and 2) reduce the toll of tobacco related diseases through improved case finding and disease management for the medically underserved population. Tobacco use remains the greatest preventable cause of death in Los Angeles County, causing approximately 35 deaths each a day making it the single most preventable cause of morbidity and mortality in the County.1 The most recent statewide data suggests that smoking among teens and young adults is increasing.1
There is compelling evidence that sustained significant investment in tobacco control can reduce tobacco use. Evaluations of comprehensive tobacco control programs implemented in California and Massachusetts have demonstrated substantial reductions in tobacco use. The goals of these comprehensive programs are: (a) preventing the initiation of tobacco use among youth; (b) promoting quitting among young people and adults; (c) eliminating non-smokers exposure to environmental tobacco smoke (ETS); and (d) identifying and eliminating disparities related to tobacco use and its effects among different population groups. The Centers for Disease Control and Prevention (CDC) recommend the following as components of a comprehensive tobacco control program.1
· Community programs to reduce tobacco use
· Chronic disease programs to reduce the burden of tobacco-related disease
· School programs
· Enforcement
· Statewide programs
· Counter-marketing
· Cessation programs
· Surveillance and evaluation
These components, in combination with policy measures, resulted in a substantial reduction in smoking prevalence in California, Massachusetts and Florida. National smoking prevalence was 30.2 percent in 1989 and dropped to 24.7 percent in 1995.1 Other benefits of the implementation of a comprehensive tobacco control program included reduction in smoking prevalence among adults and youth. In California, between 1989 and 1995, cigarette smoking prevalence dropped from 21.4 percent to a low of 15.5 percent. A similar reduction in adult smoking prevalence was noted in Massachusetts from a 1989 of 23.6 percent prior to program implementation, to 21.7 percent in 1995.1 A comprehensive analysis of cigarette smoking among 8th, 10th and 12th graders revealed that the nationwide trend of increasing smoking rates between 1992 and 1994 was slowed in both California and Massachusetts.1
The table below shows the change smoking prevalence among adults in California from 1989 through 1998. The low of 15.5 percent in 1995 was followed by a relatively steady increase in smoking. Research has indicated that reductions in funding for tobacco control programs impact smoking prevalence.1, 1 Reductions in funding for tobacco control In California correspond to the observed increase in smoking among adults.
|
Prevalence Of Cigarette Smoking In Selected Areas
| ||||||||||
|
Prevalence (%) |
1989 |
1990 |
1991 |
1992 |
1993 |
1995 |
1996 |
1997 | ||
|
Los Angeles |
21.81 |
19.7 |
18.0 |
18.01 |
||||||
|
California |
21.41 |
19.7 |
19.5 |
20.1 |
18.4 |
15.5 |
18.6 |
18.4 |
19.2 | |
Mass. |
23.6 |
23.5 |
22.5 |
23.6 |
21.2 |
21.7 |
23.4 |
20.4 |
20.9 | |
|
U.S. |
25.51 |
25.7 |
26.5 |
25.0 |
25.5 |
24.7 |
24.7 |
25.3 | ||
A comprehensive analysis of cigarette smoking among 8th, 10th and 12th graders revealed that the nationwide trend of increasing smoking rates between 1992 and 1994 was slowed in both California and Massachusetts.1 In California, recent statewide data suggest that smoking among teens and young adults is increasing.
APPENDIX FIVE
COMPARISION OF PROPOSED LA COUNTY PLAN AND CDC PLAN
CDC Recommended Components for Comprehensive Tobacco Control Programs |
CDC Recommended Annual Expenses for Los Angeles County (Minimum-Maximum)
|
FY 99-00 allocations
|
Difference with CDC Low Estimate
|
Difference with CDC High Estimate
|
Community Programs to Reduce Tobacco Use |
6.736-19.247 |
12.762 |
+6.026 |
-6.485 |
Chronic Disease Programs to reduce the Burden of Tobacco Related Diseases |
1.005-1.417 |
5.867 |
+4.862 |
+4.450 |
School Programs |
8.267 - 12.401 |
10.223 |
-38.044 |
-62.177 |
Enforcement |
4.138-7.699 |
0.501 |
-7.237 |
-43.198 |
Statewide programs |
Not applicable |
|||
Counter Marketing |
9.623-28.870 |
10.328 |
+0.705 |
-18.542 |
Cessation Programs |
0.119-20.453 |
6.647 |
+5.608 |
-12.574 |
Surveillance and Evaluation |
7.041-16.959 |
2.324 |
-5.155 |
-17.123 |
Administration and Management |
3.520-8.479 |
3.740 |
-2.207 |
-8.191 |
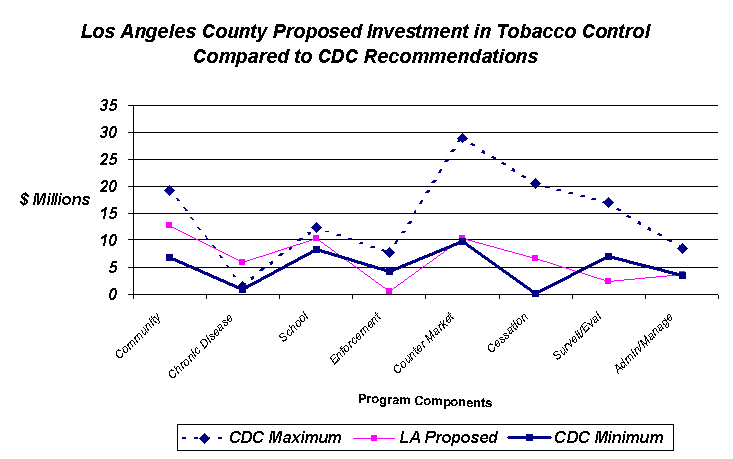
The table above compares the estimated 99-00 Los Angeles County allocation for various areas of tobacco control to CDC recommendations for a comprehensive statewide tobacco control program. The CDC estimates were applied to the Los Angeles County population. Current FY99-00 tobacco control funds (including Proposition 99 funds) were added to the proposed settlement investments to arrive at an estimated investment for each program component for Los Angeles County. These estimates were compared to CDC recommendations.
The County proposal exceeded the CDC minimum recommendations for the following components: (1) Community Programs to Reduce Tobacco Use; (2) Chronic Disease Programs to Reduce the Burden of Tobacco Related Diseases; (3) Counter Marketing; and (4) Cessation Programs. The CDC maximum recommendation was exceeded for investments in chronic disease programs.
Minimum CDC recommendations were not met for Surveillance and Evaluation, Administration and Management, School Programs and Enforcement components. It is important to note that these estimates did not include funds for statewide activities that are conducted in Los Angeles County.
Los Angeles County Population: 9,623,420
|
CDC Recommended Components for Tobacco Control Programs |
CDC Recommended Annual Expense for
Minimum - Maximum |
Los Angeles County
|
Description of Proposition 99 - Tobacco Health Education Account |
Current
|
FY 00-01 |
FY 01-02 |
MSA + Prop 99 allocation for FY 99-00 |
Difference with CDC Low Estimate |
Difference with CDC High Estimate |
I. Community Programs to Reduce Tobacco Use:
|
$6,736,394 - 19,246,840
|
$6,433,700 |
Includes all Los Angeles County funding of community based organizations, coalitions, Pasadena and Long Beach Tobacco Control Programs *excludes data from State funded competitive grantees because comparable data is not available. |
$6,328,181 |
$6,205,157 |
$2,963,246 |
$12,761,881 |
$6,025,487 |
$(6,484,959) |
II. Chronic Disease Programs to Reduce the Burden of Tobacco-Related Diseases:
|
$1,005,000 - $1,417,500
|
$5,867,400 |
None |
N/A |
N/A |
N/A |
$5,867,400 |
$4,862,400 |
$4,449,900 |
III. School Programs:
|
$48,267,028 - $72,400,542
|
None: Long-term Family Self Sufficiency and Health Student Partnerships will provide health services in collaboration with Los Angeles County schools. |
Includes Los Angeles County share of TUPE (Tobacco Use Prevention Education) funds. |
$10,223,236 |
$10,223,236 |
$(38,043,792) |
$(62,177,306) | ||
IV. Enforcement:
|
$7,738,070 - $43,698,736
|
$501,025 |
None – Prop 99 funds cannot be used for enforcement. |
N/A |
N/A |
N/A |
$501,025 |
$(7,237,045) |
$(43,197,711) |
V. Statewide Programs:
|
$384,936 – $9,623,420
|
N/A |
Statewide Tech Assistance Grants: Prop 99 funds statewide technical assistance grants that serve Los Angeles County, as well as the rest of the State; however, comparable data is not available. |
N/A |
N/A |
N/A |
N/A |
N/A |
N/A |
VI. Counter-Marketing:
|
$9,623,420 - $28,870,260
|
$2,545,969 |
LA County Media Contractors = $840,328
|
$7,782,200 |
$6,893,139 |
$6,687,200 |
$10,328,169 |
$704,749 |
$(18,542,091) |
VII. Cessation Programs:
|
$119,000 Screen only ($1 each))
|
$6,015,417 |
California Smoker’s Helpline (30%) Los Angeles County cessation program activities. |
$631,587 |
$645,431 |
$642,148 |
$6,647,004 |
$5,607,710 |
$(12,573,571) |
VIII. Surveillance and Evaluation:
|
$7,040,807 - $16,958,490
|
$1,439,575 |
Includes actual Los Angeles County evaluation costs, 10% of total allocation for LA Link, Pasadena and Long Beach. |
$884,877 |
$907,861 |
$847,368 |
$2,324,452 |
$(5,154,962) |
$(17,123,335) |
IX. Administration and Management:
|
$3,520,404 - $8,479,245
|
$1,533,151 |
Includes actual Los Angeles County administration costs, 5% of total allocation for LA Link, Pasadena and Long Beach. |
$935,651 |
$1,000,026 |
$986,365 |
$3,739,707 |
$(2,206,556) |
$(8,190,743) |
APPENDIX SIX
REVIEW OF MODEL PROGRAMS
The lessons learned from model programs reviewed in the preparation of this plan are summarized below.
Interventions Promoting Healthy Communities
· Smoking and physical inactivity are demonstrated to increase risk for common preventable illnesses1 and are accountable for a significant proportion of mortality among adults.1
· Research in California and other parts of the United States has shown that a comprehensive community-driven approach designed to change social norms is more effective in reducing tobacco use than focusing on individuals who smoke; this lesson has applications for other community health issues, e.g. alcohol use.1,1,1,1,1,1
· Promoting a decline in the prevalence of smoking, alcohol abuse, drug use, and violence will require promotion of culturally and linguistically appropriate support services and grassroots work to create policy change within the different ethnic- and gender-specific populations.1
· Emerging evidence suggests that daily physical education improves academic performance. Physical inactivity is linked to obesity, low self-esteem, and accelerating rates of hypertension and Type II diabetes in adolescents. Participation in regular physical activity is associated with leanness, tobacco and alcohol abstinence, decreased sexual activity in girls, and lower levels of violent victimization and perpetration.1,1
· Providing relevant information to legislators regarding the current scientific understanding and best practices is critical in informing their policy decisions.1
County-wide Tobacco Use Prevention Media Campaign
· Youth media campaigns that have sufficient reach, frequency and duration have been effective in reducing teen tobacco use initiation and promote teen tobacco cessation; a significant decrease in teen tobacco use has been attributed to Florida's TRUTH media campaign.1
· Children are three times more affected by advertising than are adults and are more likely to use the most heavily advertised brands.1
· Tobacco education, through paid television, radio, billboard and print advertising, promotes smoking cessation and decreases the likelihood of smoking initiation.1
· Media campaigns regarding environmental tobacco smoke issues, i.e. smoking in the home, have greatly reduced public and private exposure to tobacco smoke.1
Physical Activity Promotion Among Seniors
· Exercise studies targeting seniors have demonstrated improvements in mental ability, mood, strength, and agility associated with decreases in falls, extended independent living, and overall higher quality of life.1,1
· In one study of retirees of a large corporation, a health promotion program cost $30/participant, saving $142/participant in direct health care costs.1
Community-Based Nutrition-Physical Activity-Smoking Cessation Interventions
· Smoking and physical inactivity/obesity increase risk for most common preventable illnesses, including diabetes and congestive heart failure, two of the diseases which are a focus of the 1115 Waiver proposal.1,a,1
· Small (1-3%) decrease in dietary fat decreases first-time heart attacks by 25%.1
· Moderate (4.5%) decrease in body weight can prevent full-blown diabetes in many susceptible individuals.1
· Smoking is responsible for the vast majority of lung cancers, and contributes to heart disease, chronic bronchitis, and cancers of the mouth, throat, and gastrointestinal tract.t,u
· Effective risk reduction (physical activity, nutrition education, smoking cessation) programs can substantially cut medical costs.1,s,k
Alcohol and Depression Screening and Treatment
· Individuals with substance abuse problems and depression utilize health care services at a higher rate than others do.1
Primary Care Practice-Based Smoking Cessation Counseling
· Within Los Angeles County $1 billion per year in direct medical expenditures is attributable to tobacco use.1
· Brief advice to quit from a physician or other healthcare provider produces small but consistent increases in cessation (3-6%) after a year.x,z
Prevention Services For Juvenile Detention and Ambulatory Care Clinic Populations
· High risk youth population within which surveillance and preventative intervention should be conducted on on-going basis.1,1,1,1,1,1
· High rates of chlamydia and gonorrhea in teens, especially incarcerated youth, many of whom are poor and receive County medical services.1,1
· Untreated chlamydia results in serious and costly reproductive health consequences for women including pelvic inflammatory disease, infertility, and ectopic pregnancies (leading cause of maternal death).1,1,1,1,1
· 90% of infected adolescents do not have symptoms and therefore do not seek care.1,1,1,1,1,1,1
· Untreated sexually transmitted disease increase the likelihood of HIV infection.1,1,1,1,1,1,1,1,1
APPENDIX SEVEN
IMPLEMENTATION PLAN
The following outlines the major steps, timelines, and accountable managers for implementing the 10-year Health Improvement Strategy. The Strategy is divided into three phases: planning, program implementation, and a mid-course review and adjustment. The Strategy consists of four initiatives, each with objectives listed below in chronological order. The initiatives are (1) Prevention, (2) Early Diagnosis and Treatment, (3) Management of Diseases and Conditions (including clinical pathways, disease management protocols and case management of high utilizers), and (4) Open Door/Safety Net (including the enhancement of ambulatory care services).
Two of the initiatives, Prevention and Open Door/Safety Net, require a community-based planning process for the development of area-specific program recommendations. Allocation of resources will be based on unmet need formulas developed for each of these two initiatives. Examples of factors that may be considered for a Prevention allocation formula include population size, disease burden, the number of high-risk teens, and poverty. Factors for the Open Door/Safety Net allocation formula include distribution of unmet need for ambulatory care services, self-reported levels of difficulty in obtaining medical care, and preventable hospitalizations for selected illnesses in public hospitals.
Upon final Board approval for the Open Door/Safety Net initiative, the Department will allocate designated funds to DHS facilities and initiate a competitive bid process to identify new private partners or expand services of current providers. For the Prevention initiative, a competitive bid process will be used to solicit proposals from private agencies, as well as DHS facilities and programs, in an effort to identify the best public or private entities to provide services.
Step/Timeline |
Accountability |
1. By June 20, 2000, submit report to Board of Supervisors. |
Director of Health Services |
2. By July 31, 2000, obtain feedback from external stakeholders. This could include meetings with key individual stakeholders or stakeholder groups, SPA-based community planning meetings, and/or formal community hearings. |
Director of Public Health |
3. By July 31, 2000, develop resource allocation formulas for Prevention of Health Risks and Enhancement of the Open Door/Safety Net Systems initiatives. |
Director of Public Health |
4. By July 31, 2000, develop specific action plans for Early Diagnosis and Treatment of Remediable Health Problems and Improvement in Cost-Efficiency and Disease Management initiatives. |
Director of Public Health Chief Medical Officer |
5. By July 31, 2000, outline steps and timeline for community-based planning process for implementation of the Prevention and Open Door/Safety Net initiatives. The process will include participation of a central Planning Council and SPA-based community groups. |
Director of Public Health |
6. By July 31, 2000, submit progress report to Board of Supervisors, with: (1) description of community response to report (see Objective 2 above); (2) implementation action plans for the Early Diagnosis, Treatment and Management of Diseases and Conditions initiatives; and (3) proposed allocation formulas and proposed community-based planning process for the Prevention and Open Door/Safety Net initiatives. |
Director of Health Services |
7. By August 7, 2000, begin community planning process, with periodic updates to the Board of Supervisors. |
Director of Public Health |
8. By ---, 2000, submit finalized SPA-based plans and Countywide report to the Board of Supervisors for review and approval. |
Director of Health Services |
9. By ---, 2000, complete RFP programmatic outlines and submit to Public Health, Office of Ambulatory Care and Contracts and Grants. |
Director of Office of Planning |
Step/Timeline |
Accountability |
1. By July 31, 2000, begin implementation of the Management of Diseases and Conditions initiative in DHS hospitals and DHS/PPP facilities. |
Chief Medical Officer |
2. By August 7, 2000, begin implementation of the Early Diagnosis and Treatment initiative. |
Chief Medical Officer, Directors of Public Health and Ambulatory Care |
3. Sixty days after Board approval, develop Requests for Proposals or other appropriate formal processes to determine the public and private providers who will implement the Prevention and Open Door/Safety Net initiatives. |
Chief of Staff |
4. Ninety days after Board approval, implement the administrative, evaluation, quality assurance, and monitoring components necessary for each of the initiatives. |
Chief of Staff, Chief Medical Officer and
|
5. Implement four of the 39 clinical pathways each fiscal year with 12 pathways implemented by June 30, 2002. |
Chief Medical Officer |
6. By June 30, 2003, pilot-test all six disease management protocols with protocols for pediatric asthma and coronary heart failure piloted by January 2002, and HIV and diabetes piloted by February 2003. |
Chief Medical Officer |
7. By June 30, 2005, implement all case management programs for high utilizers. |
Chief Medical Officer |
8. By June 30, 2007, implement all six disease management protocols. |
Chief Medical Officer |
Mid-Course Review and Adjustment
A mid-course review will be conducted to (1) assess our performance in achieving the desired outcomes, (2) determine if unanticipated barriers have been identified and addressed and (3) assess the accuracy of cost figures. If needed, a revised strategy will be submitted to the Board for approval.
Master Tobacco Settlement Funds for Los Angeles County:
An Opportunity to Improve the Health of County Residents
Executive Summary
This plan responds to the Board of Supervisors’ (Board) directive to develop and recommend spending priorities for the Master Tobacco Settlement funds. As such, the plan recommends interventions and programs for use of these funds and does not address securitization or investment fund options available to the Board. Unlike many jurisdictions, the Board has unanimously voted to use the settlement funds for health improvement and health care. It has directed the Department to develop specific plans that focus on the expansion of outpatient services, indigent health care, treatment of tobacco-related diseases, expansion of tobacco education and prevention programs, and other public health priorities.
Although no formal process for input of interested parties has been completed to date, the Department did receive input during plan development through its contacts and relationships with many stakeholders and concerned parties. The Department recommends a structured process to obtain stakeholder input following the Board's consideration of this preliminary spending plan. This process would include obtaining comments from interested parties in each service planning area (SPA).
The County and its partners are faced with tremendous unmet needs for both the prevention and treatment services necessary to improve health and reduce disease. It is estimated that Los Angeles County will receive an estimated $2.7 billion over the next 25 years in Master Tobacco Settlement funds—an average of about $105 million per year. This is a reduction from the $130 million per year that had been anticipated in previous drafts of this document. This reduction is based on new computations from the State Attorney General’s Office. Nonetheless, funds from the Tobacco Settlement represent an unprecedented opportunity to advance the overall restructuring process of the Department of Health Services and to realize the public health vision of improving the health status of Los Angeles County residents.
This plan is an important building block to realize the vision for a healthier Los Angeles, one in which each person is offered the opportunity to realize their health and economic potential. Consistent with the recently released Healthy People 2010 goals, the vision includes a focus on reducing the burden of chronic diseases and reducing health disparities among different groups within the County. A major means to achieving this vision is through each individual receiving timely, high-quality prevention, diagnostic and treatment services throughout their life span. Further, realizing this vision requires that public agencies and partners work together to forge healthier communities and supportive social and physical environments.
Both prevention and treatment services are needed to improve the overall health of County residents. Thus, the vision is to improve the cost-effectiveness of our health investments through a combination of enhanced investments in cost-effective prevention, incremental expansion of services, and further strengthening of the safety net. However, even with these funds, the large and growing underserved population will still have unmet needs absent significant State and /or federal health system reform.
The majority of the burden of disease for County residents results from preventable conditions, most of them chronic, including heart disease, cancers, stroke, arthritis, diabetes, depression, cirrhosis, lung diseases, such as emphysema and injuries. There is a large body of scientific evidence indicating that these conditions are preventable to a substantial degree. One of every two deaths in Los Angles County is attributable to preventable conditions and behaviors such as abuse of tobacco, alcohol and other drugs, inadequate physical activity, poor nutrition, substance abuse, violence and inadequate early diagnosis and treatment. Successful prevention and control of these chronic conditions requires combining a variety of approaches and interventions to reduce these risk factors.
Public health restructuring has laid a foundation for implementing a comprehensive set of chronic disease prevention programs. Reinvigoration activities, started in 1998, have increased the Department's capacity in health promotion, chronic disease prevention and health assessment and epidemiology. Area health officers have been appointed to work with partners and community based organizations to implement programs responsive to community needs.
Opportunities
In developing this plan, the Department considered existing priorities that could potentially be addressed with additional revenue. These included both infrastructure and service expansion projects, which alone could exceed Tobacco Settlement funds. However, the Board's directive was interpreted as a challenge to devise a plan that would examine the broad health needs of County residents and recommend, taking into consideration other potential funding streams, the best use of these funds to significantly improve the health of the population. This plan represents our best thinking regarding the use of these funds. While not minimizing the need for revenue to support current projects, the plan makes a significant step towards a balanced approach addressing both existing service needs (e.g., capital improvements, service expansion), as well as recommending investments to reduce the burden of disease among county residents.
In the Department's recommendations, emphasis has been placed on realizing broad goals to improve the health of Los Angeles County residents. This plan focuses on accountable strategies to:
· Increase the span of healthy life for Los Angeles County residents by reducing the burden of chronic diseases and injuries;
· Reduce health disparities among various population groups and improve the distribution of available resources between geographic areas;
· Improve access to preventive services provided by the Department and its partners, that can, over time, reduce the inappropriate demands on the safety net system; and
· Monitor and evaluate the effectiveness and efficiency of these investments.
These recommendations are based on a careful analysis of major disease burden, opportunities to leverage proposed investments, and evidence about the effectiveness of interventions to reduce health risks and health disparities among different population groups. Great care has been taken to consider alternative options and opportunities necessary for a comprehensive, long-term strategy for community health improvement. Thus, Tobacco Settlement funds are targeted for areas where funding is not otherwise available and revenues can be maximized.
Major assumptions are that Proposition 10 funds and Long-Term Self-Sufficiency funds will address service gaps for their target populations. We will work with the Proposition 10 Children's and Families First Commission and DPSS to continue to ensure coordination around the needs, priorities and opportunities for intervention to positively impact the health of their respective target populations. In the event that these funding streams do not adequately address these populations and their respective needs, we will re-evaluate our recommendations.
The plan was developed under the assumption that the 1115 Waiver extension, as currently proposed, will be approved making federal matching funds available for the strategies and interventions outlined in the 1115 Waiver extension plan, including proposed amendments. Approximately $60 million of the proposed spending of Tobacco Settlement funds will be invested directly on 1115 Waiver objectives currently under consideration by HCFA and that the use of remaining Tobacco Settlement funds will also support the broad Waiver goals. A summary of the relationship between the Tobacco Settlement proposal and the proposed 1115 Waiver commitments is included in the following table.
While the average of $105 million per year is the best current estimate of anticipated funds, changes in tobacco use nationally, particularly decreases, could significantly affect future revenues and would require a re-evaluation of priorities and allocations of available funds. It is also important to note that while the plan assumes approval of the 1115 Waiver extension, it is acknowledged that significant reductions in anticipated Waiver related revenues would result in the need for re-prioritization of the use of these funds.
COMPARISON OF PROPOSED TOBACCO SETTLEMENT, 1115 WAIVER
| |||||
|
DESCRIPTION |
(A) TOBACCO
|
(B) WITHHOLD
|
(C)
NET AVAILABLE FUNDS |
(D) 1115
|
(E) NET
|
Prevention Promoting Health Behaviors
|
$13.0
|
$1.3
|
$11.7
|
IV |
$3.6 |
Subtotal |
$24.0 |
$2.4 |
$21.6 |
$3.6 | |
Early Diagnosis and Treatment of Remediable Problems (2) Smoking Cessation Depression, Alcohol and other Substance Use Screening and TreatmentSTD Prevention, Screening and Treatment |
$ 7.0
3.0 |
$0.7
0.3 |
$6.3
2.7 |
IV |
$2.7 |
Subtotal |
$14.0 |
$1.4 |
$12.6 |
$2.7 | |
Improved Service Delivery and Chronic Disease Management (CRM) |
$5.0 |
$0.5 |
$4.5 |
I |
$4.5 |
Enhancing Safety Net & Health Protection Systems Ambulatory Care Expansion
|
$40.0
|
$0.0
|
$40.0
|
II
|
$40.0
|
Subtotal |
$62.0 |
$2.2 |
$58.9 |
$49.0 | |
Other Waiver Objectives |
$0.0 |
$0.0 |
$0.0 |
$0.0 | |
Grand Total |
$105.0 |
$6.5 |
$98.5 |
$59.8 | |
Notes:
(1) In the process of identifying Waiver related adjustments included in SQ #86, Other Program Needs.
(2) May include prevention.
(3) Goals as listed in the 1115 Waiver Extension Request Project Plan approved by the Board on October 1999
A balanced investment plan includes funding for prevention, early diagnosis and treatment, expanded health services, enhancing the cost-effectiveness of care, and improvements in infrastructure to support the core mission of the Department. Four categories of health improvement opportunity have been identified that are consistent with the Board direction and represent good investments to help achieve plan goals. These are:
· Prevention of serious health risks and diseases,
· Early diagnosis and treatment of remediable health problems,
· Enhancing safety net systems, and
· Infrastructure development and capital improvements.
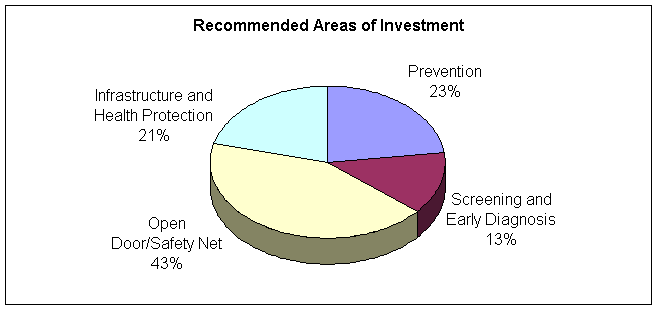
The figure shows the division of recommended funding into four major areas of investment. Two critical areas are prevention and early diagnosis and screening activities to reduce the burden of chronic disease and serious health problems among Los Angeles County residents. The focus on preventive care in clinical settings is exemplified by the recent implementation of the Office of Women’s Health Cervical Cancer Screening Initiative. This successful set of activities demonstrate how the translation of policy decisions and priorities into programs emphasizing screening, early identification and treatment can help reduce diseases disproportionately impacting sections of our population.
Significant investment is also recommended to enhance the safety net system and to expand this traditional role to that of an "open door" system, improving access to a wider range of health services. While a variety of providers (private hospitals, emergency rooms, etc.) contribute to the “safety net” of emergency services available to Los Angeles County residents, DHS and its partners also provide access to a full range of preventive and early diagnostic and treatment services. As "open door providers," DHS and its public/private blended network are moving towards an emphasis on prevention that can ultimately reduce the burden of disease on the population and the public health care system. This proposed plan will greatly advance this transformation by focusing on vulnerable populations through selective interventions and strategies.
Investments are also proposed to increase the Department's health protection capacity and to improve infrastructure. The LA Health Survey is an example of the benefits of investments to improve the Department’s capacity to assess and monitor health related issues in Los Angeles County. This comprehensive survey of County residents provides information about health needs, health care access issues and opportunities for intervention for use by the Department, its partners, and community stakeholders to plan and implement health improvement strategies and increase access in each part of the County. The LA Health Survey data has been particularly important in demonstrating the need for extension of the 1115 Waiver.
The following section provides an overview of interventions associated with each area of investment. All programs will be required to have impact/outcome and performance measures, and each intervention will include evaluation activities to assess the return on these investments. A proportion of funds, between one and five percent depending on the complexity of the program and the required evaluation, will be provided for internal and/or external evaluations.
The spending priorities outlined in this plan are consistent with the restructuring of the Department under the 1115 Waiver--building on the successes of the first five years, addressing some of the identified shortcomings, and advancing the restructuring process as outlined in the 1115 Waiver extension request. Thus, this plan recommends further expansion of ambulatory care by allocating significant annual amounts toward meeting the local match requirements to reach annual visit targets; investing in information system infrastructure, disease management, and the evaluation of specific interventions; and, ultimately, investing significant amounts in programs that reduce the burden of disease on specific populations that rely on the safety net/open door delivery system. Ten percent of the funding for prevention, early diagnosis and treatment, and capacity building and health protection interventions will be held in reserve, acting as a buffer against changes in the amount of Settlement payments and to address potential changes in priorities.
Strategy 1: Prevention of Serious Health Risks and Conditions - Four proposed interventions are designed to reduce the risks associated with chronic diseases and promote healthier behaviors among County residents. It is recommended that $24 million be allocated to implement these interventions.
Screening, early diagnosis and treatment of remediable health problems through clinic-based prevention services are essential to reduce disease burden and improve health. It is recommended that $14 million be invested in these interventions.
· Screening for tobacco use and counseling using established guidelines for physicians and other health professionals: Brief advice to quit smoking from a physician or other health care professional produces small, but consistent, increases in cessation after one year. This intervention would provide screening, counseling, and smoking cessation services to primary care patients at DHS and private partner sites. The intervention also includes partnering with private physician associations and others to train physicians Countywide. Anticipated outcomes over five years include: (1) identifying and screening 90 percent of smokers seen by open door providers; (2) provision of cessation counseling to 50 percent of smokers seen by open door providers; and (3) a decrease in smoking prevalence by 4 percent.
· Screening for STDs (including HIV) and related treatment in high risk populations and expansion of screening in ambulatory care settings: There are high rates of chlamydia and gonorrhea in teens, especially incarcerated youth, many of whom rely on County-funded health care services. The recommended interventions are: a) to screen approximately 30,000 juvenile detainees for chlamydia and gonorrhea and provide treatment for those infected, and b) expand screening and treatment to all DHS and private partner sites providing family planning services. Anticipated outcomes include: (1) decreases in STD infection rates; and (2) expanded access (number of sites) to screening and treatment services.
Strategy 3: Enhancing the Open Door/Safety Net System
The open door/safety net system in Los Angeles County, despite recent expansion in ambulatory care, is vulnerable given the large and rising needs of the uninsured and underinsured. Tobacco Settlement funds, because they provide a large revenue stream, can be used to strengthen the ambulatory care delivery system and maximize total available funds under the 1115 Waiver, providing an open door/safety net system emphasizing cost-effective, preventive care, early diagnosis and disease management for all patients.
· Ambulatory Care Enhancement: To assure access to ambulatory care and enhance the mix of services through cost-effective methods that serve uninsured patients relying on both DHS and PPPs, it is recommended that we program an average of $40 million per year. The funds would support primary and specialty care services in outpatient settings, focusing on:
· meeting the proposed 1115 Waiver-related ambulatory care commitments in the extension requirement currently under consideration by HCFA;
· integrating public health services as part of basic primary care services in ambulatory settings;
· creating financial incentives for ambulatory care providers to meet a full range of established, age-appropriate screening and assessment prevention guidelines; and,
· enhancing quality assurance and systems for the evaluation and monitoring of the quality of care and of population based services.
· Infrastructure Development: To promote systems integration across the delivery system and empower clinicians, planners, administrators, epidemiologists and others to directly manage, monitor, evaluate, and report on patient care and population health status, it is recommended we invest $10 million in additional funds for information system technology and training. Fifty percent of this amount would be invested in clinically based projects that improve clinical record keeping to track and evaluate patient care. The other 50 percent would be invested in population based systems for a data warehouse, web-based application to facilitate information exchange with county residents, health care providers and a wide range of public and private organizations, enhancement of disease surveillance, and other data projects to track progress in meeting health goals and increasing accountability.
· Capital Improvements: To significantly upgrade and expand facility capacity for ambulatory care, it is recommended that $12 million per year be targeted for capital improvements. These funds would be used to guarantee repayment on capital construction, supporting approximately $150 million in capital spending based on the priorities in the Board- approved DHS capital plan that also considers the needs of the PPPs as part of the DHS system. Capital improvements could include building/refurbishing of physical facilities. Expected outcomes are more cost-effective, integrated delivery of health and other human services, and increased use of DHS and PPP facilities by patients with health benefits.
The table below presents the proportions of investment for each proposed intervention. An annual average of $105 million is anticipated over the 25 years of the settlement. Using the $105 million per year figure, the proposed plan includes significant investments in interventions addressing tobacco control, chronic disease management, and chronic disease prevention and control. Tobacco use prevention and control activities are represented in both prevention and early diagnosis and treatment interventions and are estimated to represent an investment of approximately 15 percent of total Settlement funds.
Because of the initial 1998-1999 payment, funds will remain from the first year of plan implementation. Currently $135 million has been received for 1998/1999 and 2000 periods for application to the $105 million proposed spending plan. While $10 million of this will be held in reserve for 2001, during which a $95 million payment is anticipated, the remaining $20 million will be available for one-time-only use. In addition, due to first year start-up, as much as $10 million may remain unexpended. Funds from these two sources will total $30 million for one-time-only funding for a variety of Board priorities.
Overview of InterventionsProportion of Total Settlement Funds Allocated to Proposed Interventions | |||||
|
INTERVENTIONS, CATEGORIZED BY AREAS OF OPPORTUNITY FOR IMPROVEMENT (Proposed allocations assume $105 million annually.) |
Prevention In Clinical Care Delivery |
Tobacco Prevention And Control |
Chronic Disease Prevention |
Capacity & Infrastructure |
Recommended Spending Allocation
|
PREVENTION (23%) |
|||||
· Promoting Healthy Behaviors ($13 M) |
X |
X |
12% | ||
· Mobilizing Communities for Health ($2 M) |
X |
X |
2% | ||
· Reducing Tobacco Use ($5 M) |
X |
X |
5% | ||
· Promoting Physical Activity Among Seniors ($4 M) |
X |
4% | |||
EARLY DIAGNOSIS AND TREATMENT OF REMEDIABLE PROBLEMS (13%) |
|||||
· Smoking Cessation ($7 M) |
X |
X |
X |
6% | |
· Alcohol/Drug Use and Depression Screening and Treatment ($4 M) |
X |
X |
4% | ||
· STD Prevention, Screening and Treatment ($3 M) |
X |
3% | |||
ENHANCING OPEN DOOR/SAFETY NET SYSTEMS (43%) |
|||||
· Ambulatory Care Enhancement ($40 M) |
X |
X |
X |
38% | |
· Cost Effective Management of Diseases and Conditions ($5 M) |
X |
X |
X |
5% | |
STRENGTHEN CAPACITY AND IMPROVE HEALTH PROTECTION (21%) |
|||||
· Infrastructure Development ($10 M) |
X |
10% | |||
· Capital Improvements ($12 M) |
X |
11% | |||
TOTAL FUNDS |
100% | ||||
I. A $24 million annual investment per year in prevention interventions that promote healthy behaviors, mobilize communities for health, and reduce tobacco use.
II. A $14 million annual investment per year in the early diagnosis and treatment of remediable problems through clinic-based prevention services for smoking cessation, alcohol and substance abuse screening and treatment, depression screening and treatment, and sexually transmitted diseases screening, prevention, and treatment.
III. A $45 million annual investment to enhance open door/safety net systems and cost-effective disease management strategies by expanding ambulatory care services and implementing incentives for the provision of high quality preventive services.
IV. A $22 million annual investment to strengthen and improve capacity and health protection systems by upgrading facilities and better monitoring and reporting on the health of individuals and populations.
V. It is recommended that ten percent of the funding for interventions in the areas of prevention, early diagnosis and treatment, capacity building and health protection enhancements be held in reserve to address potential changes in priorities and serve as a buffer against future funding reductions.
The strategies, types of interventions, fund amounts, and implementation plan are outlined in the body of the report. A series of mid-course reviews and reassessments are included at five year intervals as a part of plan implementation. This review will be informed by ongoing evaluations that will comprise an integral part of each intervention.
The plan requires the Department to continue working with its partners, including other County departments, private health service providers, free and community clinics, health care organizations, community based planning and health improvement groups, local academic institutions, labor, consumer advocates and other community representatives. By working together in our many communities, the funds invested from the Tobacco Settlement Agreement can greatly enhance efforts to achieve both improved health status of Los Angeles County residents through investments in prevention and in a strengthening of the open door/safety net system in an accountable fashion.
Other jurisdictions may be interested in securing Tobacco Settlement funds to address needs within their communities. In developing this plan, we examined the health needs of all County residents, thereby including the residents of the 88 cities within the County. Consequently, the interventions proposed will benefit city residents. We anticipate that some cities may wish to apply for funding when RFPs and other processes for allocation of funds are initiated.
Two phases of reporting are envisioned following approval of this preliminary plan:
· Reporting during development of Implementation Plan: Following approval of this plan, detailed action plans will be developed for each set of investments. During this initial period we will return to the Board of Supervisors every 90 days with a report of progress in developing action plans, interventions and processes to allocate funds both internally and externally. A detailed implementation plan will be prepared to describe program and intervention rollout.
· Reporting following development of Implementation Plan: Following completion of the implementation plan, we will return to your Board quarterly to report on program and intervention progress. Implementation progress reports will include descriptions of processes used to engage the communities and stakeholders in program planning and implementation and timelines, as well as results of competitive bid and other allocation processes. Progress reports will also include descriptions of methods developed to monitor program implementation, as well as periodic reports of program milestones. When appropriate both process and outcome measures will be reported, however it is anticipated that initial reports will be limited to process and intermediate outcome measures.
Intervention project reports will be required for all areas of investments. To ensure accountability performance measures will be established for each program and will be included in semi-annual progress reports along with current expenditures.
We envision a process to obtain stakeholder input on this plan that would include a series of stakeholder meetings, a written report of stakeholder comments, and presentation of the report to the Health Planning Council to obtain their advice and recommendations. Using the Department's extensive database of community stakeholders, organizations, providers and advocates, a series of Service Planning Area based meetings will be held. Input will also be gathered during upcoming meetings of stakeholder groups with Countywide representation and employee forums at DHS facilities. For consistency, all stakeholders will receive the same presentation, and will be asked to respond to a set of specific questions.